|
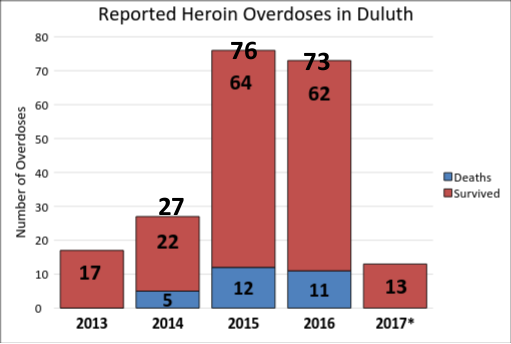
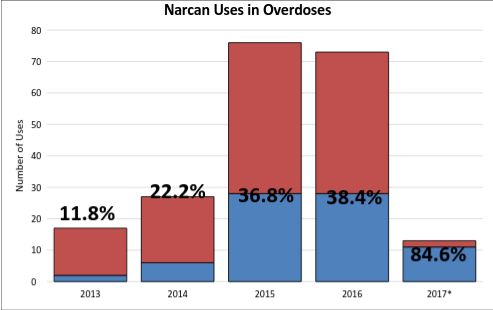
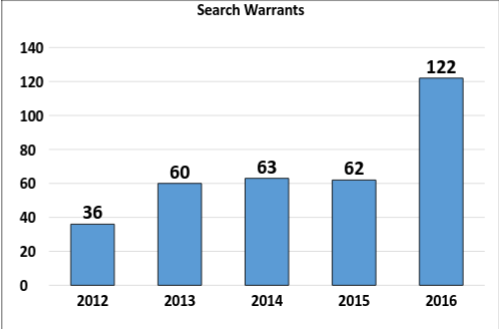
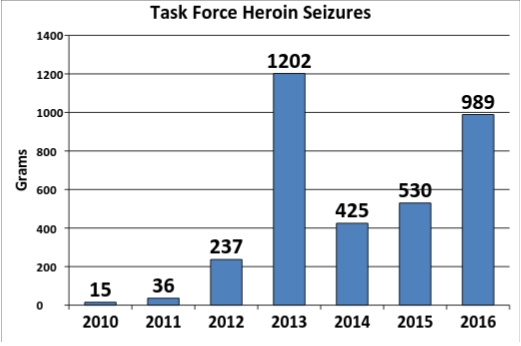
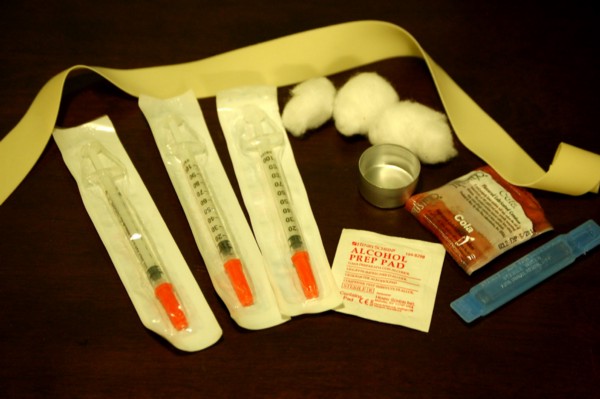
by Max Reagan & Ben McDonald Duluth Mayor, Emily Larson, mentioned in her State of the City address last month that tackling the opioid addiction problem is a priority for the city. “St. Louis County has the highest per capita rate of opioid-related drug overdoses in the state,” said Larson during her address. “Higher even than Hennepin and Ramsey counties.” In response to this endemic ravaging the Northland, Larson announced the creation of an opioid withdrawal unit, stating that Duluth will work with St. Louis County, the Center for Alcohol and Drug Treatment, and the 6th District Judicial Court. The unit would support users and make sure resources are available for recovering from addiction as a way to make Duluth a more livable for its citizens. St. Louis County is just one of many areas following this nationwide trend of increasing deaths from opioid overdoses due to legal prescriptions such as Oxycontin and Dilaudid as well as illegal drugs such as heroin. But how did this happen? Why have opioids become such a problem not only for Duluth but the nation as well? How Opioids Have Become Such a Problem: Prior to the 1990s, the majority of opioid prescriptions were given for severe post-surgical pain or end-of-life treatment. According to an Associated Press article, Painkiller Politics, during the 1990’s, opioids began being used to treat chronic pain after pharmaceutical companies and some medical experts claimed they could be used without addiction — these claims proved to be misleading. Justina Brusacoram, a emergency service technician at Essentia Health — St. Mary’s Medical Center, witnesses the destruction of opioid misuse on a weekly basis. “The problem is that the pharmaceutical industry has created an addiction to opioid pain medication,” Brusacoram said. “Which has led to patients further seeking of drugs like heroin.” Brusacoram attributes the increased use of heroin in this area as a result of prescription medications. When patients who have been receiving opioid pain medication for chronic pain can no longer receive these pain medications they turn to illicit drugs such as heroin. It may be easier and cheaper to obtain. “The people that we are seeing having overdoses in the ER, which are a very frequent thing, they are not the typical junkies that you’d expect to see on the street using heroin. It is your everyday mom and pops, grams and gramps coming in with overdoses,” Brusacoram said. This is a problem that is not restricted by social barriers, but runs rampant in all social classes and all parts of society. Another part of the problem is the over-prescribing of these medications by physicians. Brusacoram says this could be due to a negative outcome of the Affordable Care Act that switched compensation for hospitals based on services provided to compensation based on outcomes and patient satisfaction surveys. One component of this patient satisfaction survey is pain management. “Now doctors are rated on their quality based on their patient satisfaction scores,” Brusacoram said. “We are seeing increasing pressure on doctors to prescribe pain management medications to avoid negative scores on HCAHPS.” Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) is the name of the patient satisfaction scores that determine the amount of funding a hospital receives. How Big is the Problem? What Are the Numbers?: As of April 2017, Duluth has seen 13 reported overdoses. According to the statistics provided by the Duluth Police Department, there has been a 329 percent increase in reported overdoses from 2013 to 2016 (Fig. 1). With the increase in reported overdoses has also come an increase in the use of Narcan (Fig. 2), a medical injection that has the powers of reversing an opioid overdose. The percentage of time that Narcan is administered in overdose reports has also increased from 11.8 percent in 2013 to 84.6 percent through March of 2017. Also on the rise has been the number of search warrants issued and executed by the Duluth Police Department Drug Task Force as they have been searching to eliminate the source of the heroin (Fig. 3). From 2015 to 2016, there was a 97 percent increase in the number of search warrants executed by the Task Force, increasing from 62 to 121 — more than doubling the previous year’s totals. The amount of heroin seized in Duluth has also followed this trend (Fig. 4). Task Force heroin seizures have increased from 2010 to 2016, having seen a 6493 percent increase in the amount of heroin seized from 2010 to 2016, from 15 grams to 989 grams. A Look at the Opioid Withdrawal Unit: The opioid withdrawal unit would be a joint venture between the city of Duluth, St. Louis County, the Center for Alcohol and Drug Treatment, the 6th District Judicial Court, and local hospitals. The unit would be a safe place for those who overdose to receive immediate care. Currently it can take sometimes up to a week for a user to be admitted into a hospital. It would also aid those who wish to medical intervention to assist in the withdrawal from opioids. And finally, and perhaps most importantly, the opioid withdrawal unit would provide a connection to other support and resources for those battling addiction. Recovering addict Simon Ramirez-Williams discussed his experience with opioids and the creation of an opioid withdrawal unit.
“Oh I’ve done just about any substance you can think of,” Ramirez-Williams chuckled. “But heroin is the one that really took me down.” A native of San Antonio, Ramirez-Williams said that his experiences with heroin withdrawals were the worst thing he has ever endured. “I’ve been shot and sliced, but when I first went through [opioid] withdrawals that was the worst shit of my life,” said Ramirez-Williams. Simon wishes he had access to a resource like the opioid withdrawal unit during his battle with opioids. “The first time I was really off the stuff [heroin], was when I was in jail,”said Ramirez-Williams. “I went through the whole withdrawal experience alone in a cell and I told myself I would never go through this again.” Unfortunately for Simon, this was not be his last encounter with heroin. “So I was off it [heroin] for about five months until I got out [of jail] and right when I got out I went back right on my bullshit,” said Ramirez-Williams. “Doing the same stuff, hanging with the same people and sure enough within a couple weeks of being out I was right back to using.” An all too familiar story says Kira Sheldon, a social worker with the St. Louis Public Health & Human Services Department. “Without some sort of support system, relapse is almost a certainty,” says Sheldon. This is where the creation of an opioid withdrawal unit could find its greatest effect. Within a unit like this Sheldon says, “users could find support and have access to other resources for recovering from addiction.” In Conclusion: How can Duluth become a more livable city? A livable city doesn’t just entail food diversity, walkability, or a strong local economy. Perhaps the biggest thing that makes a city livable is the residents. A factor of livability can be a community of people who are willing to help out a neighbor in need, which is at the heart of the creation of this withdrawal unit. Duluth has been hit by the opioid endemic, which has brought addiction, crime, overdose and death to shores of Lake Superior. There are people in this city struggling with addiction because the resources they need are not available to them. The creation of this unit would add to Duluth’s livability in a much more literal way — it would change lives. Livability at its foundation means a city taking every necessary step to ensure the health, safety, and survival of every one of its inhabitants.
0 Comments
Leave a Reply. |
|